What is Dialysis?
Dialysis is a treatment that removes excess water, solutes, and toxins from the blood. It is also known as renal replacement therapy. The first successful dialysis treatment was performed in 1943. There are several types of dialysis. These include peritoneal dialysis, Hemodialysis, and the use of an artificial kidney.
Hemodialysis
Dialysis treatment removes excess fluid and waste products from the body. The process works by passing the blood through an artificial kidney surrounded by a membrane. The membrane permits the waste products and fluid to pass while the remaining fluid is pumped out and discarded down the drain.
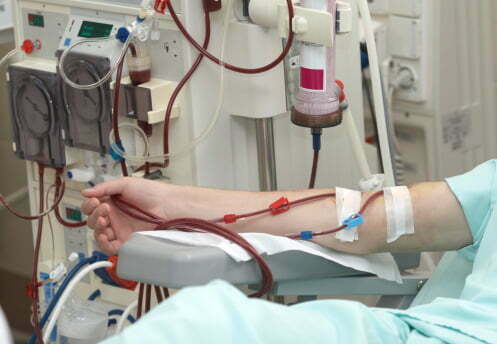
Dialysis is usually performed in a hospital or dialysis clinic but can also be done at home. During the procedure, two needles are inserted into the patient’s arm and connected to a plastic tube. This tube allows the cleansing fluid to enter the blood. During the treatment, the patient may take a nap or continue his or her normal daily activities.
The dialysis machine removes excess fluid from the blood and filters it. The filtered blood is pumped back into the patient’s body through tubes. These tubes are connected to needles inserted into a large vein or artery. The process is called vascular access, and the patient may undergo several access procedures.
Peritoneal dialysis
Peritoneal dialysis involves using the peritoneum (the membrane that exchanges fluid with blood in the abdomen) to remove excess fluid, correct electrolyte problems, and remove toxins from the blood in patients with kidney failure. This procedure is a life-saving treatment for kidney failure.
Your doctor will place a catheter in your abdomen and train you to use it. You will spend at least three hours a week prepping and cleaning your peritoneal dialysis supplies. You can get more information about the length of treatment from your health care provider. Peritoneal dialysis requires a peritoneal catheter and a cycler machine. During peritoneal dialysis, the patient will use these machines to remove excess fluid.
Peritoneal dialysis is not without risks. The most common complication is infection. Bacteria can enter the body through the catheter and connect to other organs. When an infection develops, the patient may experience pain, swelling, and redness at the exit site of the catheter. Antibiotics are added to the dialysis solution to prevent these infections. Antibiotics also help prevent hernias, an abnormal weakness in the muscles of the abdominal cavity.
Hemodialysis with a temporary catheter
In patients with acute kidney failure, hemodialysis with a temporary catheter is an important treatment option. This catheter is placed into the patient’s veins and exchanges blood with the hemodialysis machine. This method conserves venous access and minimizes invasive procedures.
The procedure is not without risks. Temporary catheters may lead to infections, decreasing dialysis adequacy and resulting in higher mortality and morbidity. It may also cause significant discomfort and cost. Moreover, patients with temporary catheters may not receive the same level of care as patients with permanent catheters.
In a study by the Renal Epidemiology and Information Network (REIN) in France, 53,092 adult patients were included. Patients were included if they had vascular access before dialysis, but patients without this access were excluded. The patient’s first visit date was used to estimate the duration of pre-dialysis nephrology care before the hemodialysis treatment started.
The central venous catheter (CVC) is the most common vascular access for hemodialysis. It is the preferred access for patients with emergent or urgent HD. According to the National Kidney Foundation’s Clinical Practice Guideline, less than 10 percent of chronic HD patients should use tunneled dialysis catheters. In 2004, the Centers for Medicaid and Medicare Services launched the Fistula First Breakthrough Initiative.
Hemodialysis with an artificial kidney
Hemodialysis with an artificial kidney is performed to treat kidney failure. This treatment involves placing two needles into the patient’s body. The first needle drains blood, and the second transport the blood to the artificial kidney. The artificial kidney cleans the blood by filtering the blood through hollow fiber tubes. These fiber tubes are semi-permeable and have small holes that mimic a kidney. As the patient’s blood flows through the fiber tubes, it moves from one end of the artificial kidney to the other.
Patients who need hemodialysis will typically require two to three treatments a week. These sessions are generally performed until a patient can receive a kidney transplant. These treatments are vital in maintaining blood pressure levels and can greatly extend a patient’s life. However, patients should not opt to refuse treatment, as this can lead to complete kidney failure and the need for a transplant.
Dialysis sessions are performed under the supervision of qualified specialists in a hospital setting. These sessions last between three and five hours with an artificial kidney apparatus. This artificial kidney pumps blood out of the patient’s artery and delivers it to the filtering system, which is cleaned with a dialysis solution.