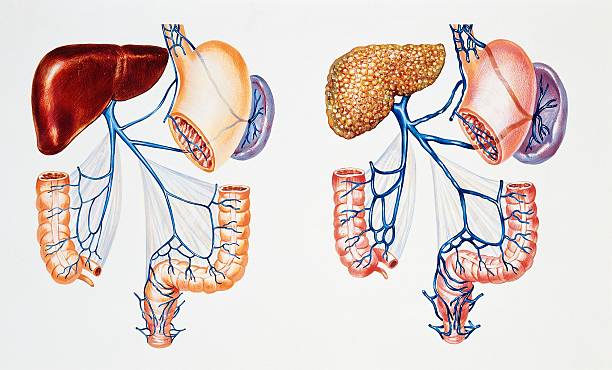
Fatty Liver Disease
Fatty liver disease is caused by a buildup of fat in the liver. Blood tests will help doctors diagnose the disease. These tests may include liver function tests, a blood count, and imaging tests. A liver biopsy can confirm the diagnosis and assess the severity of the damage. A biopsy is also an excellent way to determine the type of fatty liver disease you have.
Alcohol-induced fatty liver disease
Alcohol-induced fatty liver disease is caused by ethanol-induced dysfunction of the liver. The ethanol metabolism causes increased levels of acetaldehyde and dicarboxylic acids in the liver. Alcohol also impairs the function of PPAR-a, a protein involved in the breakdown of fatty acids.
Although it has been suspected that a fatty liver is caused by excessive alcohol intake, this disease’s exact mechanism is unknown. However, alcohol-induced fatty liver disease is one of the most common causes of liver dysfunction. Alcohol consumption is associated with a high prevalence of cirrhosis and other complications, while non-alcoholic people tend to develop only minor or no liver disease.
Alcohol consumption increases the production of certain hormones and inflammatory proteins in the liver. These include glucagon, interleukin-1, and interleukin-8. The adipocytes secrete a peptide known as adipokines, which regulate hepatic lipid metabolism. Alcohol-induced fatty liver disease likely results from complex interactions between the different cell types in the liver. In addition, ethanol doses can increase oxidative stress, mitochondrial dysfunction, and peroxisomal dysfunction.
Fibrosis
Although many people have NAFLD, only a small percentage will have severe liver disease or even experience fibrosis. For this reason, noninvasive tests are preferred for an initial assessment. However, many of these tests are subject to false-positive results, especially in patients with advanced diseases. To prevent false-positive results, clinicians should consider confounding factors in interpreting the results of these tests.
Imaging-based liver CT (pCT) can be used to detect the presence of fibrosis. It is a high-resolution imaging technique that captures changes in tissue perfusion during fibrosis. It is typically performed after administering an intravenous bolus of contrast agent. The images are then processed to determine quantitative or semiquantitative tissue perfusion parameters.
Cirrhosis
Although cirrhosis and fatty liver disease are not fatal, the symptoms of both can be devastating. Liver cancer occurs in about 10% of patients with cirrhosis. The liver is unable to produce enough proteins and may eventually fail. This condition can cause jaundice and even scarring.
Symptoms of fatty liver disease include weight loss, itching, and yellow skin. Fatty liver disease can lead to cirrhosis, a more severe disease if not treated. If untreated, cirrhosis can lead to liver failure and life-threatening complications. Diagnosing fatty liver disease usually involves blood tests and imaging. A liver biopsy can also be performed to diagnose fatty liver disease.
Fatty liver disease is characterized by the accumulation of fat cells in the liver. A similar condition called cirrhosis is characterized by the development of scarring over the healthy parts of the liver. Both types of fatty liver disease can lead to cirrhosis, but cirrhosis is much more severe.
Treatment
Although there is no specific medication for fatty liver disease, treatment options focus on controlling factors contributing to the condition. Your doctor will likely prescribe a diet and exercise plan to help you maintain a healthy weight and improve your metabolism. He may also prescribe medications to control your blood sugar, cholesterol, and triglyceride levels.
A doctor can diagnose fatty liver disease by performing blood and imaging tests. These tests can rule out other liver disorders and identify the extent of fatty liver damage. A liver biopsy may also be done to look for inflammation and scarring.